Relapse #2 & Lung GVHD
Chapter 3 :
2014 – 2015
2014
Relapse, CAR T-Cell and BMT #2
Home only 11 months, I began to experience that lower back pain that I was all too familiar with.
Local blood tests were inconclusive and after talking to my doctors at St. Jude, I was told to fly back immediately the next day.
A bone marrow biopsy revealed my biggest fear, my leukemia had returned. Call it naive but I thought it was not possible to relapse after a bone marrow transplant.
I cried, and my family cried. There was nothing we could do but face this head on. – Again.
The Protocol
BiTE Trial, Chemotherapy, CAR T-Cell and BMT #2
Over the years I had developed an immunity to many of the chemo drugs and some couldn’t be given at all as they are toxic and I had already reached my life time limit. A third cancer diagnosis was definitely a problem.
I would be given new and more intense drugs to outsmart the leukemia cells.
May - BiTE Trial
A new trial drug (approved in 2015) was offered to me called: The BiTE Trial – Bispecific T-cell Engager.
The drug Blinatumomab was infused over 24 hours a day, for 28 consecutive days. It reduced my cancer cells by half, not the number needed to head into transplant.
My doctor would now use her expertise to develop a tailored chemotherapy protocol to suit my needs.
Fact: I had to write a sentence of my choice in handwriting everyday twice a day to determine if there was neurological damage.
This drug could not be turned off for longer than 2 minutes when switching bags.
June - Intensive Chemotherapy
June 9th started the hardest chemotherapy I have ever done. Many complications arose such as C-Diff, typhilitis, liver and kidney problems. These in turn need their own set of medications which have their own side effects. Drugs, for drugs, from drugs.
As tough as everything was, my doctor reassured me things were moving in the right direction. No matter what was thrown at me or how awful I was feeling, the program was working and I was thankful for it.
July 17 - 0.02%
The chemotherapy protocol was finished and my leukemia was reduced to 0.02%. Given my circumstances and history, this was an incredible result! At this point I could go straight into my second bone marrow transplant, but because I relapsed after my first transplant, we wanted that number to be 0.00%.
The Next Step:
A new treatment was discussed called CAR T-cell (Chimeric Antigen Receptor T cell Therapy). It had the potential to wipe out any remaining cancer cells and offered at just a few hospitals in the USA. We chose Seattle children’s hospital in Seattle, WA. They were starting a new trial and welcomed me into their program.
As a Canadian I would have to pay out of pocket for this expensive trial, but it was worth the chance to be cancer-free.
Seattle , Wa
Seattle Children's Hospital
Seattle Chilren's Hospital
July 26
Moved to Seattle, WA for CAR T-Cell Thearpy At Seattle Children’s Hospital
I would be the 10th patient to receive this new treatment!
Phase 1 - August 6
My T-cells were removed by apheresis and taken to the lab for 2-3 weeks for modification. making them able to bind to cancer cells and kill them.
Chemotherapy would continue to keep my cancer at bay and weaken my immune system further so the new t-cells would be more easily accepted.
Phase 2 - September 16
Millions of my new engineered T-cells were ready to be infused back into my bloodstream!
Phase 3 - September 22
I experienced a mild cytokine storm with massive headaches and mild fever requiring hospitalization for 12 days. I was very fortunate to have a “mild storm” because when immune cells are activated they release large amounts of cytokines into the body causing increased inflammation which can be life threatening.
October 8
After 64 days, my cancer was gone 0.00%! MRD negative. It worked!
Minimal residue all disease is a term used to describe the small number of cancer cells in the body after cancer treatment. An MRD negative result means that no disease was detected after treatment.
My Thoughts On... CAR T-Cell Therapy
This process is incredible. Besides the chemotherapy I had to keep doing, the Car T-cell therapy was minimal and an easy compared to my other past treatments. Because I felt well enough throughout, I was able to explore Seattle, eat at restaurants (trying my best to follow the low bacteria diet haha), shop, and even attend my first NFL football game, Go Seahawks!
After going through so much the last few months it was the break I needed to get me through what was to come.
Back to St. Jude
& Bone Marrow Transplant #2
November 10
After Seattle I flew back to St. Jude for Bone Marrow Transplant #2.
The difference between my first BMT and second was that my mom would be the donor. This is called a haplo transplant. Unlike my first transplant where I received just one bag of donor stem cells, this time I would receive multiple bags of stem cells over a one week period.
Haploidentical transplant: Is a half matched stem cell transplant from a family member – parents, siblings and sometimes even cousins. Based on genetics it will always be half a match.
Because only one parent is 50% of me, the risk of getting GvHD (graft vs. host disease), is much higher.
November 21
I was admitted into the BMT ward for my Second Bone Marrow Transplant. I started the Conditioning Phase where I underwent chemotherapy to destroy cancer cells and surpress the immune system to prepare the bone marrow for the new stem cells, and given chemotherapy to further weaken my immune system and make room for my new cells. My mom who was going to be my donor was going through the donor collection process:
The donor receives daily injections of growth factor to increase stem cell production. The donor’s cells are collected through apheresis, separated for the patients needs and infused later that same day.
Unlike the first BMT where I was given one unit of my donors stem cells all at once, the haplo process collects six units of stem cells over six days from the donor.
On the last day, Day 6, is the NK cell infusion, Natural Killer Cells
December 1
Bone marrow transplant day! I waited almost 9 months in preparation for this very day.
However this being my second time going through this process made it all the harder. I knew what to expect and knew hard days where just ahead.
I had many complications over the month but was well enough to be released after 42 days on Christmas Eve.
However, on Christmas Day,
Into the I.C.U
During my BMT I had mild rattling in my chest and some difficulty breathing. As it worsened, I was admitted into the ICU and diagnosed with Pneumonia.
This was serious. Having little to no immune system my doctors weren’t sure if I was going to make it.
I was sedated and chest tubes were inserted to drain the fluid from my lungs. The rest of my family traveled to join my mom and everyone took turns watching over me 24/7.
2015
Recovery, Home to Canada & New Diagnosis
January 2nd - I turned 18 in the I.C.U.
Being sedated allowed my body to rest while the antibiotics tackled the pneumonia infection. As more fluid drained from the lungs my condition started to improve and I eventually moved back to the regular BMT ward.
Over the Next 5 Months... I celebrated many victories and dealt with many downfalls.
This being my second BMT and an allogenic transplant (50% match from from my mom), I encountered many more problems and side effects than my first one.
Anti-Depressants
At the beginning of my 3rd cancer diagnosis I was put on antidepressants knowing the long road that lay ahead. After trying different types and brands over the months, I was having adverse reactions like mood swings, aggression, hallucinations and even depression. All these dealings added a new layer of hardship and my experience with them caused more harm than good.
Mysterious Illness
At the end of April I developed a painful condition. The skin on my hands and feet was bright red and peeling. The inside of my mouth and esophogus was inflamed with sores and my lips were swollen and blistered. Many doctors came in to have a look… but none had any idea what this was. The closest diagnosis was Lepracy. The pain was EXCRUCIATING but thankfully the condition subsided after a few weeks.
Gallbladder Removal
June, seven months after my transplant I developed GvHD of the gut/GI track. Sharp pain in my abdomen and back, bloating, diarrhea, nausea/vomitting and weight loss led to my doctors ordering a HIDA scan. I was put on oral medications to treat the GvHD and had surgery to remove my Gallbladder.J
Small Victories
I also had good days and celebrated small victories!
I stopped my TPN (liquid food infusion) after many months, and my liver biopsy was negative for GvHD.
WARNING
GRAPHIC PHOTOS – HOVER TO REVEAL
heading...
HOME!
As my body healed and got stronger over the months, the complications and side effects lessened. I was approaching the time to be discharged from St. Jude and be seen on an outpatient basis!
Although this was amazing news, it was difficult in many ways. Not only was I nervous to live so far away from my medical team, I worried about the possibility of relapsing. It was an odd feeling to think I’d return home and “back to normal” after what I had just gone through. I had to remind myself as hard as everything had been, I was lucky to be alive. So many pass away from cancer and they fought just as hard.
To celebrate the news of going home, my mom, sister, and I ate at the Peabody Hotel, saw the famous duck walk and ended the night with a carriage ride!
Home To Canada
August 1st
1 year and 4 months since my treatment started I was able to return home to Canada!
I was happy to be back home but disappointed to miss my high school graduation by just one month. From the start of treatment this was always my goal. This would have been the last time to see the people I grew up with, be in their photos and have a great night together. Instead, I had to watch it all happen on social media.
Treatment is hard, but so is missing out on life.
During my time at home I was able to “catch up” on my life. I went to my first bar and drink (legally) as well as gamble at the casino! Although I missed out on so much, I was grateful to be home and ready to re-start my life!
GvHD of the Lungs + Lung Biopsy
December
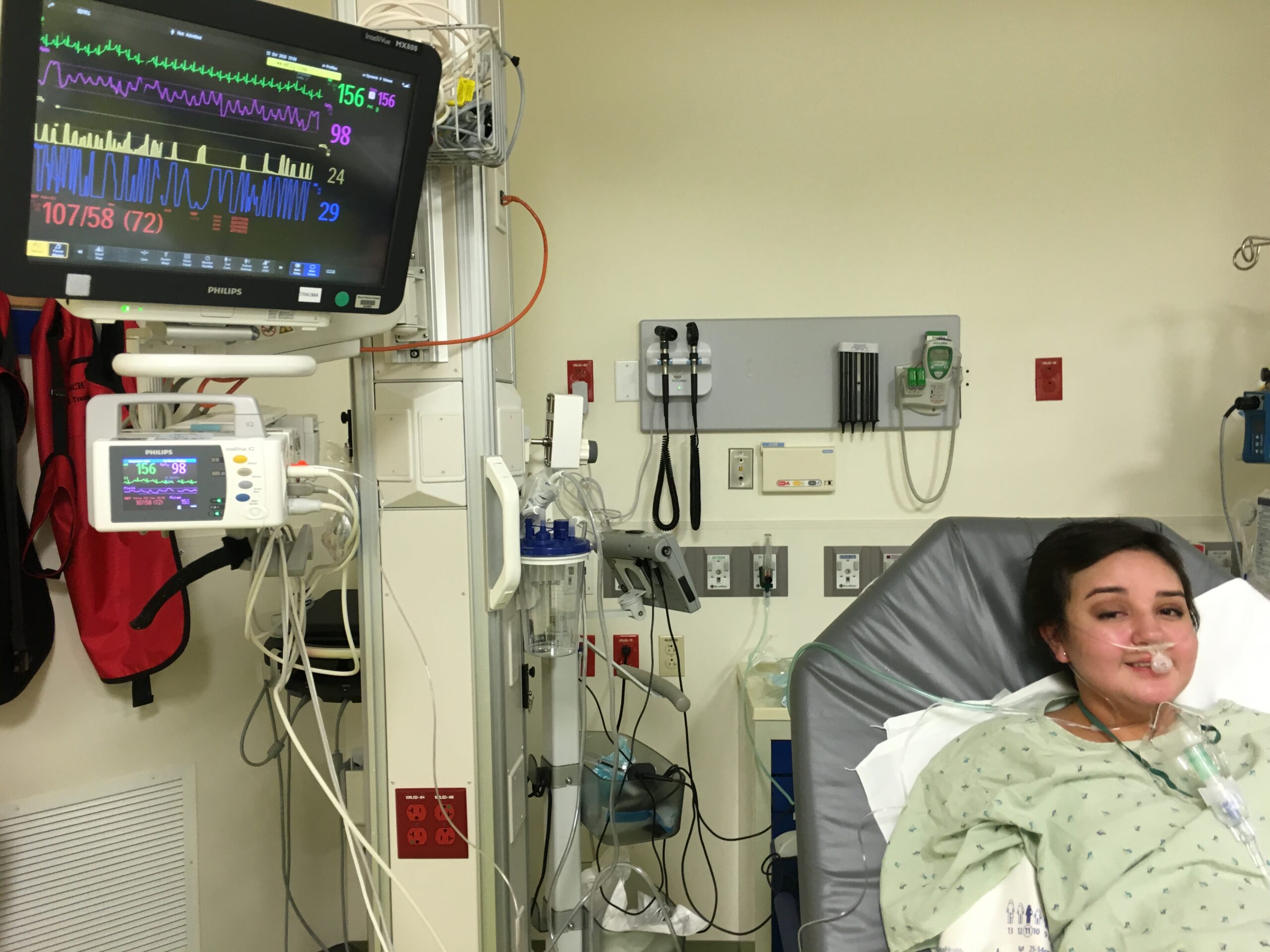
Back at home I continued having breathing difficulties. This affected my heart rate as it got dangerously high several times reaching over 160BPM. Twice during the month an ambulance was called to take me to the Emergency Room.
The staff Respirologist requested a lung biopsy.
December 11th I was officially on home oxygen and my lung biopsy results revealed I had GvHD of the lungs.
After my biopsy I developed a pneumothorax (a collapsed lung) and code blue was called. Because of this I would spend my 3rd consecutive Christmas + birthday in hospital again.
Reflecting on a new Diagnosis:
After a year of conquering cancer and having a second bone marrow transplant, I thought the hard part was over. It was devastating to know I now had a completely different disease - lung disease.
With my GvHD diagnosis I was constantly breathless doing ordinary tasks like walking and bending over. Being put on home oxygen was a scary reality of how serious this was. Not only did I feel disappointed for myself but especially for my family. They all witnessed me at my worst in the last two years and I really believed after the BMT that we would get to make up for lost time. Instead of traveling and celebrating, we were all frustrated and hit a breaking point.
That being said, we tried to keep our spirits high and remained hopeful that this would resolve. We frequently went to the casino, saw hockey games (Go Oilers!), and played BINGO at the local centre.
Trouble in Paradise
After an October check up at St. Jude, I went on my first vacation in many years to visit my sister in Miami. Three days into the trip, I had difficulty breathing and a high fever. I was admitted into Miami Children’s Hospital ICU for the next 12 days. When my condition was not improving my doctor arranged for me to be medivac’d back to St. Jude Hospital.
Once landed, I was admitted into the ICU and sedated. Fluid was drained from my lungs and antibiotics were started. My brother, sister and dad flew in and took shifts watching over me… just like the last time I had pneumonia in 2014. Over 5 weeks I slowly recovered and returned back home to Canada
What is GvHD:
GvHD occurs when the donors t-cells (graft) view the patients healthy cells (host) as foreign they attack and damage them.
The more mismatched your donor is, the higher chances of developing GvHD.
GvHd can be mild, moderate or severe (acute or chronic).
Acute: Commonly happens within first 100 days after transplantation
Chronic: Can occur anytime after transplant or several years after transplant
Important Note: GvHD can have some benefit, developing it means that while your “new donors cells” are attacking your healthy cells, they are also destroying any surviving cancer cells. Patients who develop GvHD have lower relapse rates.
My GvHD Experience:
Acutely, I had GvHD of the gut/GI track 4 months after my second bone marrow transplant. My skin and liver were biopsied but both were negative for GvHD.
Chronically I now had GvHD of the lungs and also of the eyes.
With my first BMT I never developed any GvHD and had relapsed. With my second BMT and having so much GvHD I felt comforted knowing the new cells were inside of me, working to create a new immune system.
Ready for More?
Diagnosed with Lung GvHD, Moving to Toronto, Lung Transplant & Stroke